Grateful Patient Stories
If you would like to share your donor story, we would love to hear from you. Donor stories inspire our medical staff to continue to do what they do. They also inspire other people to donate to your hospital and impact many other patients.
-

Coral’s Story
For more than six decades, Coral has had a home at Blue Mountain. While she no longer skis herself, the mountain continues to bring her connection and joy. From the comfort of her home, she watches the skiers of Blue Mountain make their way down the slopes. This had become a lovely pastime for Coral throughout the winter…
-

Jay’s Story
Jay Richardson splits his time between Toronto and South Georgian Bay and has owned a home in the area for more than 25 years. Over the years, this community has become an important part of his life. Seven years ago, after a biking accident, Jay was brought to CGMH for an assessment. During what could…
-

David’s Story
David Barrett is a charismatic, lively family man whose passion for skiing and golfing keeps him healthy, happy, and fit. When he started having a series of headaches that wouldn’t go away, he thought this was quite unusual, and brought it up with Dr. Richard Cornell, his family physician, who promptly ordered a CT scan…
-

Barry’s Story
Carolyn and Barry have called Wasaga Beach home for nine years, having enjoyed a peaceful retirement after Barry’s career at Ontario Hydro until February of 2024 brought a health scare they never saw coming. It started with a high fever. Barry assumed it might be COVID-19 or the flu, so he and Carolyn made a…
-

Stacie’s Story
Stacie Smith grew up in Toronto and moved to Collingwood with her husband 10 years ago. They first started coming up on the weekends, to enjoy the outdoors. They love cross country skiing, mountain biking and paddling. Eventually, they decided this was the right place to live and raise their family. A few years after…
-

Judi’s Story
As a local real estate agent and long-term resident of Wasaga Beach, Judi Dosne already knows the power of community and the importance of a good neighbour. So when she recently needed care at CGMH, she was relieved and grateful to find such a supportive network that cared for her compassionately, every step of the…
-

Mark’s Story
Mark & his family have a cottage in Wasaga Beach, where they spend their summers. Almost fifteen years ago, in one of those hot summer days, Mark suffered a terrible accident and badly injured his leg. He was brought to CGMH by ambulance and Dr. Koo was tasked with trying to stich his leg back…
-
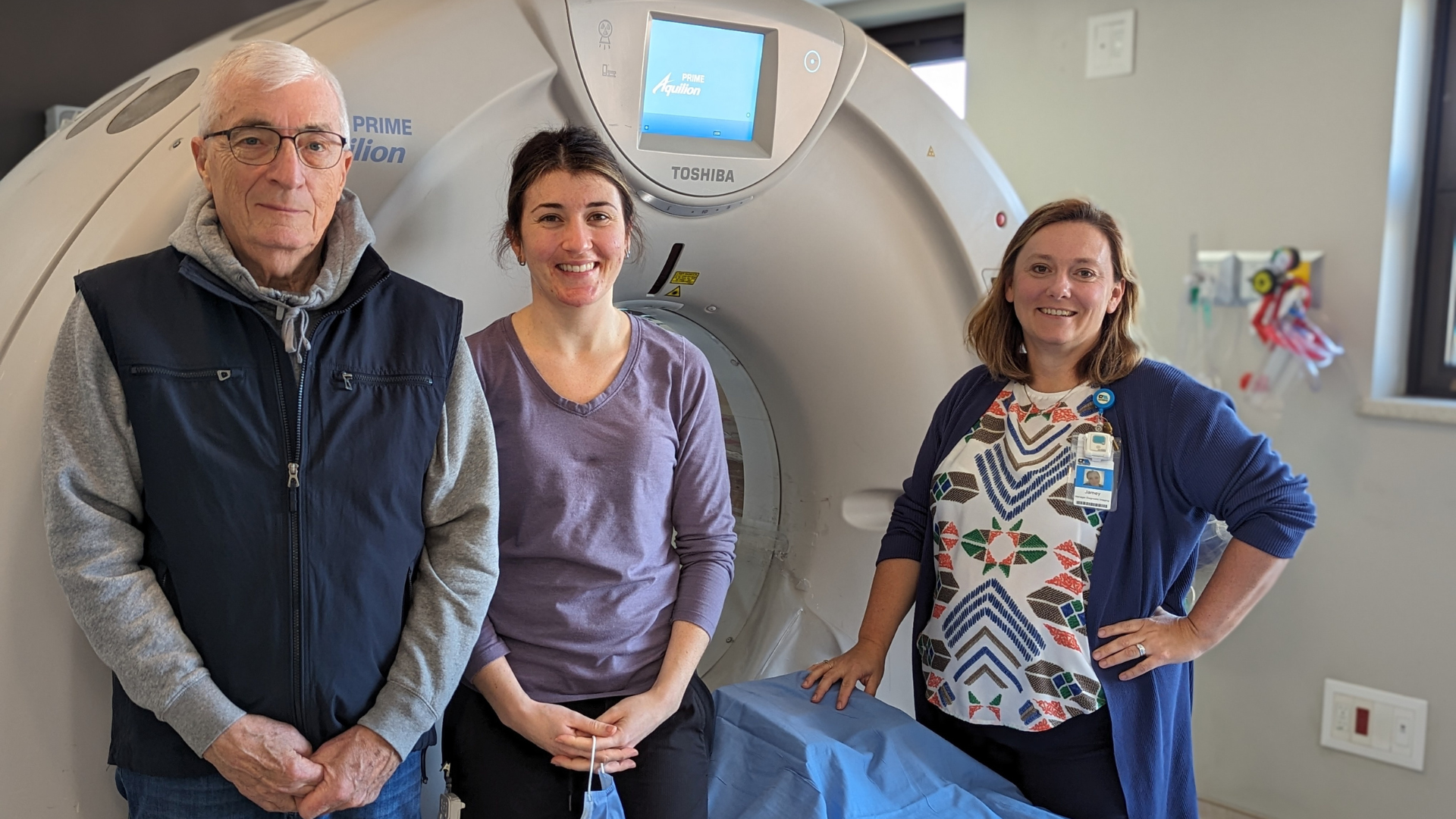
Bruce’s Story
In the summer of 2022, Bruce & Teresa Poirier decided to downsize and move from their hometown of Montreal to Wasaga Beach, as a way to be closer to their daughter and grandchildren. Almost two years in, they are very happy with the choice they made. “We love everything about living here,” say the Poiriers. …
-
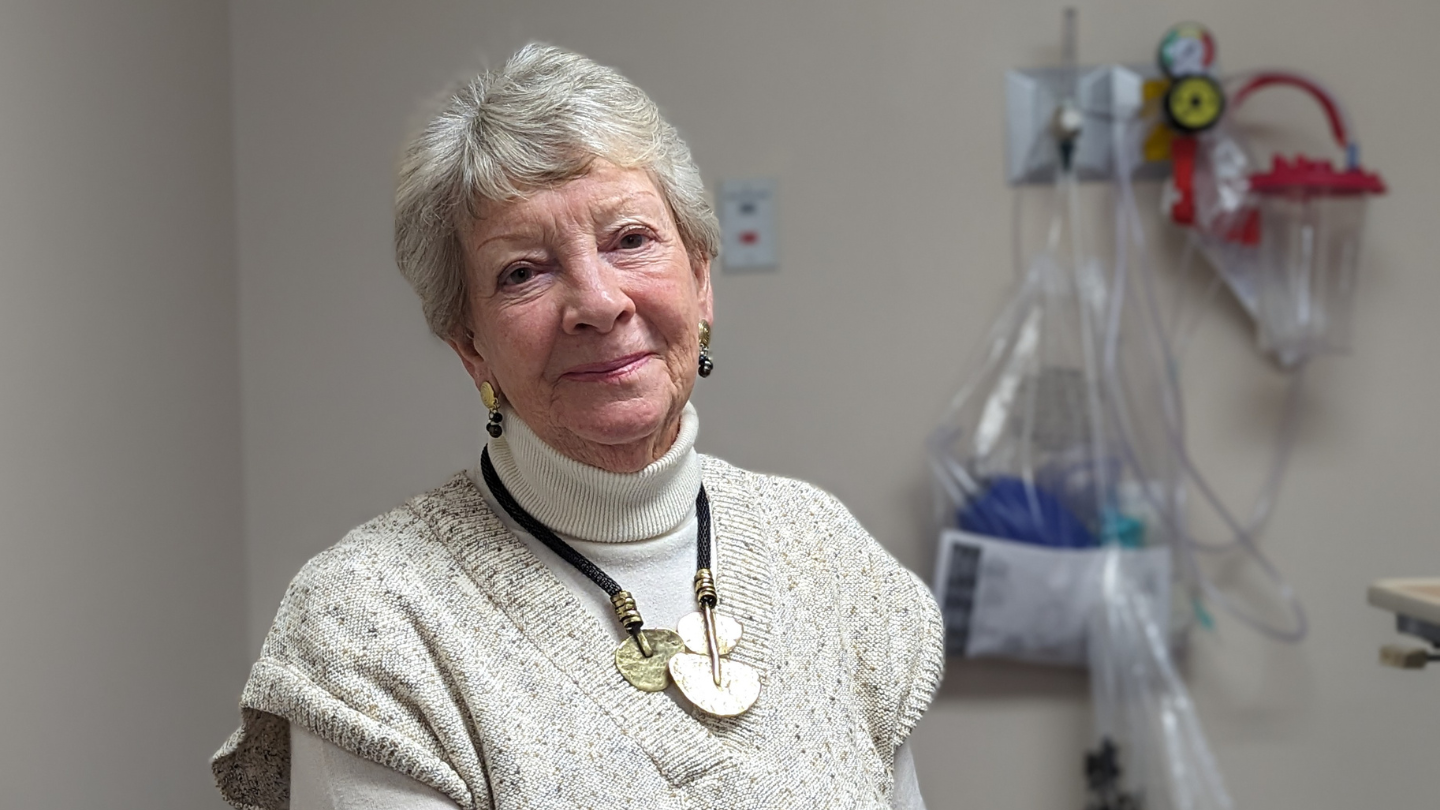
Pat’s story
My introduction to CGMH began in July when I was having trouble getting air with any kind of exertion. I went to the Emergency Department and after blood tests and an ECG proved to be fine. Dr. Jeff Matte ordered a chest x-ray, which showed a pneumothorax in the left lung. Within 45 minutes, he…
-

David’s Story
“We are always grateful to have a hospital nearby when it is needed, but the real difference lies in the people who staff it. And it is not just in their professionalism and expertise, it’s in their caring and understanding under the most demanding of circumstances. And might I add, their incredible patience. I experienced…
-

Nora’s Story
At 85 years old, Nora, a longtime Collingwood resident, found herself in a moment of crisis—rushed to the Collingwood G&M Hospital, unconscious and in urgent need of care. Thanks to the swift action and expertise of the emergency team, Nora’s condition was quickly diagnosed, and it became clear that emergency surgery was her best chance.…
-

Ellie’s Story
“This summer I was very sick for 5 weeks, getting weaker every day. My family physician, Dr. Richard Cornell ordered 3 or 4 blood tests to try to pinpoint what was wrong with me, and they showed a very high number for inflammation. So, Dr. Cornell and my partner Larry thought that I should be…
-

Mike’s Story
Moving to a new community means a lot of adjustments. After recently relocating to Collingwood, Mike Doyle’s first encounter with the CGMH was for a knee replacement and he was not sure what to expect. His experience reassured him that he could expect outstanding health care at his new local hospital. “I was so impressed…
-

Alex’s Story
November 14, 2022 began like a typical Monday for Alex. His energy levels were down after a bout with the flu a week before, but he felt otherwise fine. By mid afternoon, however, he was experiencing upper back pain and left work early. Within the short drive home, he spiked a fever and his condition…
-

Art’s Story
When a skiing accident landed Art Church in the CGMH Emergency Department, he was glad that he could be referred to Orthopaedic Services where expert surgeon, Dr. Henry Koo took over his care. To show his appreciation to Dr. Koo and the entire surgical team, Art decided to make a gift of $1 million to…
-

Jax’s Story
The Davenports moved to Collingwood to be close to CGMH Three-year old Jax Davenport has been rushed to the emergency department over 115 times. Born with a heart condition called Supraventricular Tachycardia (SVT), Jax has an irregularly fast/erratic heartbeat (arrhythmia) that affects the heart’s upper chambers. When Jax starts to feel unwell, her parents have…
-
Jim’s Story
Jim Pearse went to bed at 10 PM on a warm summer evening not feeling very well. His stomach was in pain, and he took an anti-acid to see if he would feel better. A couple of hours later, he was up again – that pain had gotten worse. Jim thought it could be an…
-

Ron’s Story
Ron Wilson has spent weekends skiing at Devil’s Glen since 1980. When he retired in 2013 he moved to the Collingwood area permanently, with the goal of golfing in the summer and skiing in the winter with his wife, Lesley. His life had been hospital free, except for when his wife gave birth to their…
-

Serena’s Story
“In September 2020, I was getting my backyard ready to watch an outdoor movie on our projector. I was carrying chairs from our deck to the lawn and missed one step! I landed hard on my right ankle and knew something was horribly wrong. I did not want to go to the hospital for fear…
-

Bob’s Story
Bob and his wife Lynn have been Collingwood residents for 20 years now. They are originally from Port Credit and have known each other since the days they played in the sandbox, at their kindergarten. Prior to moving permanently to South Georgian Bay, Bob & Lynn had been skiing in the area since the 1950s.…
-

Terry & Marilynn’s Story
Terry Reid and his wife Marilynn decided to leave their busy Toronto life behind and retire in South Georgian Bay. They now spend their days travelling the world, visiting with their 10 grandchildren, skiing in the winter and golfing in the summer. If you met them today, you would say that they are a happy…
-

Rita & Peter’s Story
We’re Rita & Peter Premich, born, raised & married in small town, Saskatchewan. Rita was blessed to be living directly across the street from the only doctor for miles around, lucky enough to have a tiny rural type hospital practically in her backyard, while Peter & his farming family, had a hard time accessing crucial,…
-

Barry & JoAnn’s story
Barry and JoAnn Suitor are soon celebrating 27 years of marriage. They are both grateful for every day they get to spend together. Life has thrown both of them some curve balls but they were always able to surpass every challenge, with a healthy dose of positivity combined with the most amazing care from the…
-

Eddie’s Story
On Sunday, June 7, 2020 I needed Emergency Room Treatment. From check in to send off many hours later, I was treated with care and respect for all my needs. It was an afternoon of Nurses’ questions, Doctors’ examinations, x-rays, ultra-sounds, more examinations and an egg salad sandwich. The professional Medical Team diagnosed the issue,…
Share your story with us!
Donor stories inspire our medical staff to continue to do what they do. They also inspire other people to donate to your hospital and impact many other patients.

Stay up to date with our latest news and upcoming events.
We promise to never spam your email and you can unsubscribe at any time.
Select an image to get started.





